Doctors and nurses probably use these words a lot if you’re taking care of an elderly parent or trying to stay healthy after getting a diagnosis. Understanding what’s the difference between ADLs vs IADLs can really affect how you plan for care, even though they sound clinical. It’s one of those differences that doesn’t seem like a big deal at first.
The short answer is: ADLs, or activities of daily living, are simple chores that people do to take care of themselves, such as bathing and eating. Instrumental Activities of Daily Living (IADLs) are harder tasks, such as cooking or managing money. Both are important, but they show different levels of independence and need different kinds of help.
What Are ADLs?
ADLs, or Activities of Daily Living, are the basic self-care tasks a person needs to physically survive and stay clean. These are the foundational skills we learn in childhood, like bathing, dressing, and eating. When someone can’t do these independently, they typically need hands-on physical assistance.
Think of ADLs as the floor of independence. If someone can’t manage these, daily life becomes physically unsafe without help.
The six core ADLs, based on the Katz Index of Independence in Activities of Daily Living (developed by Sidney Katz in 1950), include:
- Bathing washing and drying the entire body
- Dressing choosing clothes and putting them on, including buttons and zippers
- Toileting getting to the toilet, using it, and cleaning up
- Transferring moving from bed to chair or room to room
- Continence controlling bladder and bowel function
- Feeding chewing, swallowing, and using utensils
One thing worth noting: there’s a real difference between doing an ADL and doing it safely. Someone might be able to walk to the bathroom, but if they’re losing balance along the way, that’s a red flag. Falls are the leading cause of traumatic brain injuries in older adults (CDC, 2023). Don’t brush those near-misses off.
What Are IADLs?
Instrumental Activities of Daily Living (IADLs) are more complex tasks that include planning, memory, and judgment. These aren’t about staying alive. They are about living on your own in the real world. Taking care of money, cooking meals, and taking care of drugs are all examples of this.
ADLs are the floor, and IADLs are the stairs. You need them to go through each day on your own, yet they ask a lot from your brain.
In 1969, Dr. Lawton and Brody added IADLs to the original ADL framework since they knew that measuring merely basic self-care didn’t give a full picture of a person’s independence.
Common IADLs include:
- Managing finances paying bills, budgeting, avoiding financial scams
- Medication management taking the right dose at the right time, coordinating refills
- Meal preparation planning, cooking, and safely storing food
- Shopping selecting items, making purchasing decisions, completing transactions
- Transportation driving safely, using public transit, or arranging rides
- Housekeeping laundry, dishes, vacuuming, and home maintenance
- Communication using phones, email, and the internet to stay connected
A sobering statistic: in 2023, adults over 60 lost a combined $3.4 billion to fraud (National Council on Aging, 2023). Difficulty managing IADLs like finances isn’t just inconvenient. It can be dangerous.
ADLs vs IADLs: The Core Differences
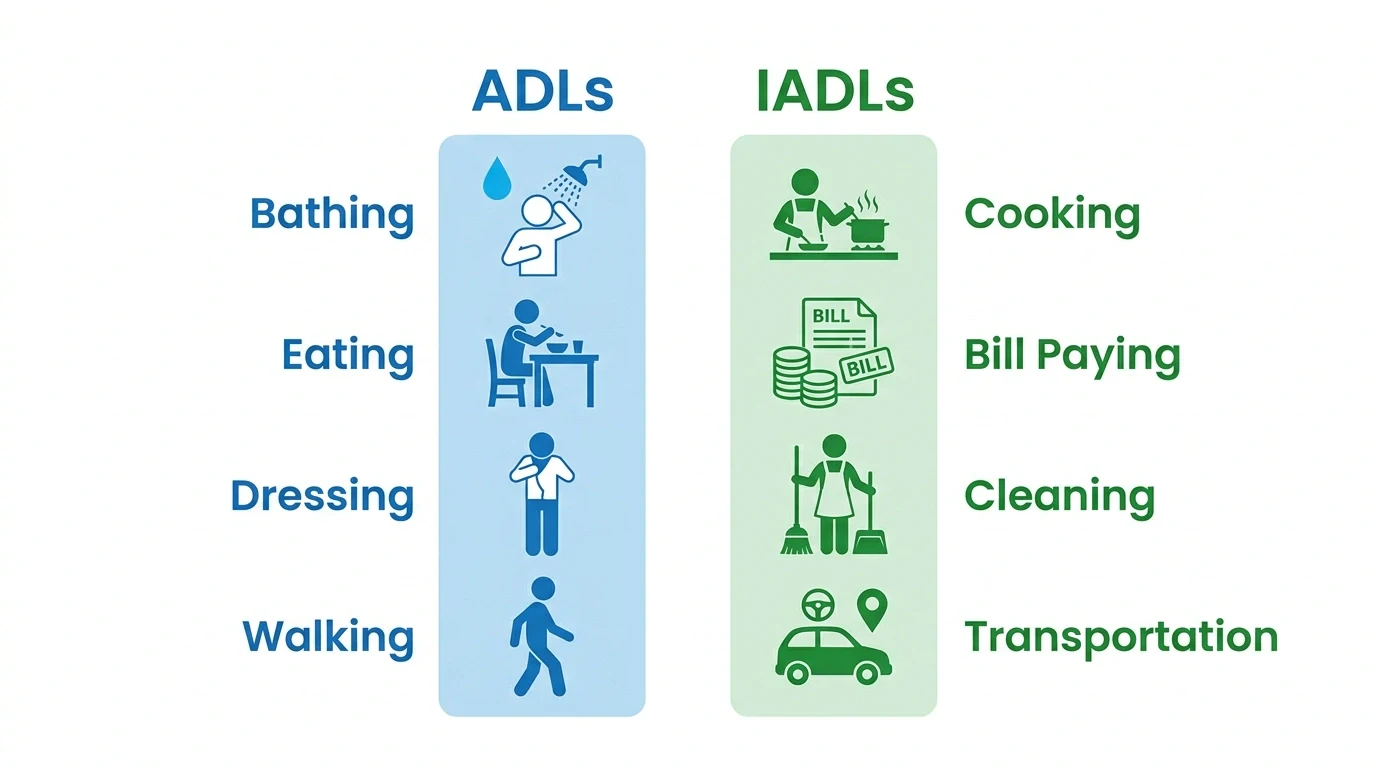
Here’s where it gets practical. Understanding what’s the difference between ADLs vs IADLs isn’t just academic. It shapes what kind of help someone actually needs.
| ADLs | IADLs | |
| Complexity | Basic physical tasks | Complex cognitive tasks |
| Examples | Bathing, eating, dressing | Cooking, budgeting, driving |
| Skills involved | Motor function, physical ability | Memory, judgment, planning |
| Who helps | Home health aides, nurses | Family caregivers, care managers |
| When they decline | Later in cognitive decline | Earlier, often a warning sign |
The biggest practical difference: IADLs tend to slip first. Someone with early-stage Alzheimer’s disease or mild cognitive impairment (MCI) might still bathe and dress themselves just fine, but start missing bill payments or forgetting to take medications. That pattern matters a lot for diagnosis and care planning.
According to the DSM-5, the primary dividing line between MCI and dementia is whether cognitive decline interferes with IADLs. This is a clinical distinction that has real implications for treatment and care decisions.
Why IADLs Matter More Than Most People Realize
IADLs often decline before ADLs in conditions like dementia and Alzheimer’s disease. This makes them an early warning system. Catching IADL decline early gives families and providers time to put support in place before a crisis hits.
Research shows that a change in IADL function may predict a dementia diagnosis within the next few years (Cloutier et al., 2020). That’s not a small window. That’s a chance to plan.
Consider this: 77% of adults over 50 say they’d prefer to age in their own home rather than a nursing facility (AARP, 2021). But aging at home safely requires someone to notice when IADLs start slipping, not just when physical care needs become obvious.
Also worth knowing: each decline in ADL or IADL function for a dementia patient added nearly five extra hours of monthly caregiving on average (Alzheimer’s & Dementia, 2024). That’s a direct impact on families.
Which Comes First: ADL or IADL Decline?
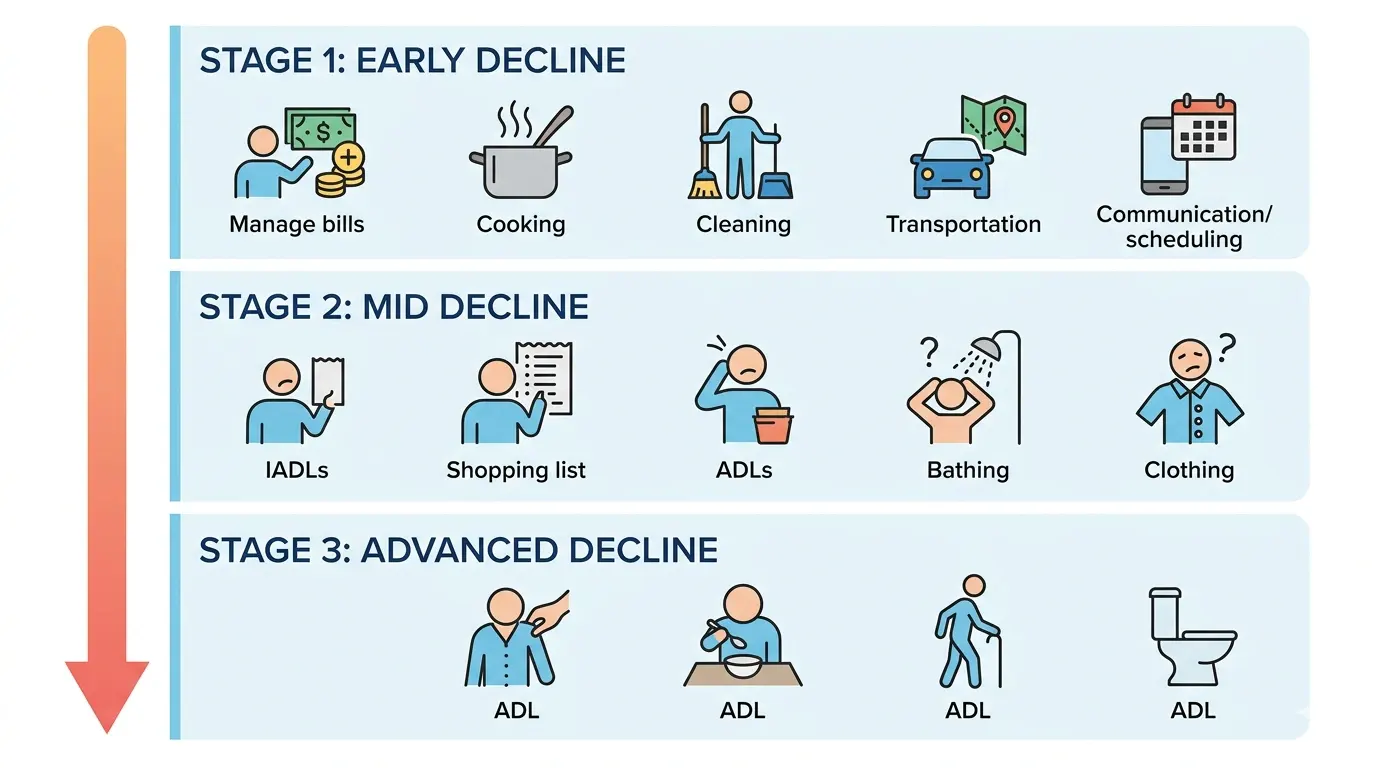
In most progressive conditions, IADLs decline before ADLs. Think of it like a river eroding a bank. The edges go first.
Someone with early cognitive decline might:
- Forget to pay bills on time
- Struggle to follow a recipe they’ve made for years
- Get confused using public transportation
But still be able to shower, get dressed, and eat meals without any help.
As the condition progresses, basic ADLs become harder too. By the time bathing and dressing are affected, a person has usually been struggling with IADLs for quite a while.
This progression is why healthcare providers, especially occupational therapists, don’t just assess someone once. They track both ADLs and IADLs over time.
Tools for Assessing ADLs and IADLs
Two primary tools are used by clinicians:
The Katz ADL Scale is based on the six core ADLs that were mentioned before. A person gets one point for each task they can complete on their own. The highest score is 6. A score of 6 signifies full independence, whereas lesser numbers show different levels of need.
The eight IADLs listed above are all included in the Lawton Instrumental Activities of Daily Living Scale. It employs a scoring system that is comparable, although the old version was known to be biased against males (it didn’t count housework and cooking when judging men). Most current doctors utilize a newer version that works for everyone.
Usually, these tests take between 15 and 30 minutes. Occupational therapists commonly do them by either watching the person directly or talking to family caregivers. Use an online checklist as a guide, but make sure to talk to a real healthcare professional about what you see. Checklists are not diagnoses; they are tools.
The Montreal Cognitive Assessment (MoCA) and the Saint Louis University Mental Status (SLUMS) exam are two more cognitive tests that are typically used with ADL/IADL tests.
What to Do When ADLs or IADLs Start to Slip
When someone starts struggling with what’s the difference between ADLs vs IADLs in real life, practical support matters more than perfect medical terminology.
For IADL struggles:
- Automated medication reminders or pill dispensers
- Grocery delivery or meal prep services
- Bill payment assistance or financial power of attorney
- Weekly housekeeping support
For ADL struggles:
- Shower grab bars and non-slip mats
- Adaptive utensils for eating
- Part- or full-time home health aide for bathing and dressing
If in-home support isn’t enough, skilled nursing facilities provide 24-hour care for complex medical needs and full ADL assistance.
If you’re based in Colorado and looking for local support, Castle Pines Home Care offers personalized home care services in Denver and surrounding areas. Their team helps families find the right level of assistance, whether someone needs light IADL support or more hands-on daily care.
Frequently Asked Questions
What is IADL in medical terms?
IADL stands for “Instrumental Activities of Daily Living.” It means doing hard things that need thinking abilities, like taking care of money, cooking, and managing prescriptions. Healthcare professionals utilize IADL tests to find out how well someone can live on their own.
What does ADLs mean in medical terms?
ADL stands for Activities of Daily Living. These are basic physical self-care tasks, including bathing, dressing, eating, toileting, transferring, and continence. They form the foundation of functional independence.
Which is an instrumental activity of daily living?
Managing finances, preparing meals, shopping, driving, and taking medications correctly are all IADLs. These tasks require judgment, memory, and planning, unlike basic ADLs which are primarily physical.
Can someone need help with IADLs but not ADLs?
Yes, and it’s actually common. People in early-stage dementia or with mild cognitive impairment often struggle with IADLs while still managing basic self-care tasks independently.
How often should ADLs and IADLs be assessed?
There’s no fixed schedule. Most providers assess ADL and IADL function at annual wellness visits, after hospitalizations, or whenever there’s a noticeable change in a person’s behavior or independence. Routine cognitive testing for patients over 65 can be billed under Medicare during annual wellness visits.