When you come into a clinic, everything looks neat and tidy. But looking clean and being safe are two entirely different things. Bacteria, viruses, and fungus are all pathogens that can’t be seen and can live on surfaces for longer than most people think. That’s why doctors and nurses use tried-and-true, science-based ways to make sure that equipment is safe before it comes into contact with another patient.
So, why are heat and alcohol used to disinfect medical equipment? The short answer is that both kill or eradicate hazardous bacteria, but they do it in different ways and with distinct methods. Heat eliminates infections by breaking down their proteins, whereas alcohol tears down their cell membranes. They serve a lot of different disinfection demands in hospitals, clinics, and homes.
Why Is Heat Used in Disinfecting Medical Equipment?
Heat is used to disinfect medical equipment because high temperatures destroy the proteins and cell structures that microorganisms need to survive. This makes heat one of the most reliable and widely trusted sterilization methods in healthcare. It works on a broad range of bacteria, viruses, and spores without leaving any chemical residue behind.
Think of it like cooking an egg. Once the protein denatures from heat, it can’t go back to its original form. The same thing happens to bacteria and viruses when exposed to high enough temperatures.
There are two main types of heat used in medical settings: dry heat and moist heat (steam). Moist heat, delivered through an autoclave, is the most common because steam penetrates surfaces faster and more effectively than dry air. Dry heat is used for items that can’t tolerate moisture.
Why Is Alcohol Used in Disinfecting Medical Equipment?
Alcohol is used in medical equipment disinfection because it breaks down the lipid membranes of bacteria and viruses, causing them to collapse and die. It works quickly, evaporates without leaving residue, and is safe for a wide range of surfaces. Isopropyl alcohol (70%) is the most commonly used concentration in healthcare.
The “70%” part matters. Pure alcohol (100%) actually evaporates too fast to be effective. The water in a 70% solution slows evaporation, giving the alcohol more time to penetrate and kill.
When it comes to sterilization alcohol, two types dominate: isopropyl alcohol and ethyl alcohol. Both disrupt microbial cell membranes and denature proteins. And yes, does alcohol kill fungus? Alcohol is effective against many fungal organisms, including Candida, which is commonly found in clinical environments.
How to Use Heat and Alcohol to Disinfect Medical Equipment
Using the right method the wrong way still leads to failure. Here’s what proper use actually looks like:
For heat: Equipment must be cleaned before sterilization organic matter (blood, tissue) blocks heat from reaching all surfaces. Once clean, items go into an autoclave or dry-heat oven at the correct temperature and for the right duration.
For alcohol: The surface must also be pre-cleaned. Apply alcohol with a clean cloth or wipe, and let it sit for at least 30 seconds. Don’t wipe it off immediately, contact time is what does the work.
A common mistake is rushing the process. Whether you’re using heat sanitize methods or alcohol wipes, skipping steps is where contamination risks sneak back in.
7 Different Ways to Use Heat and Alcohol When Disinfecting

Medical equipment disinfection isn’t one-size-fits-all. Here are seven practical methods used in real healthcare settings:
- Steam Autoclave Uses pressurised steam at 121–134°C. Best for surgical tools, stainless steel instruments, and reusable medical devices.
- Dry Heat Oven Operates at 160–180°C. Used for glassware, powders, and metal tools that can’t handle moisture.
- Boiling Water A basic moist heat method used in low-resource settings. Effective for heat-stable equipment at 100°C for at least 20 minutes.
- Isopropyl Alcohol Wipes (70%) Quick disinfection for non-porous surfaces like stethoscopes, blood pressure cuffs, and bedside rails.
- Ethanol Spray Used on hard surfaces and equipment handles. The alcohol in medical uses here is ethyl alcohol, commonly at 60–80%.
- Alcohol-Based Pre-Op Skin Prep While not equipment disinfection, it’s the same principle applied to patient skin before procedures.
- Flash Sterilization (Rapid Autoclave) A fast steam cycle used in emergencies when instruments are needed immediately. Not a substitute for full sterilization but used when time is critical.
How Heat and Alcohol Fight Bacteria and Viruses
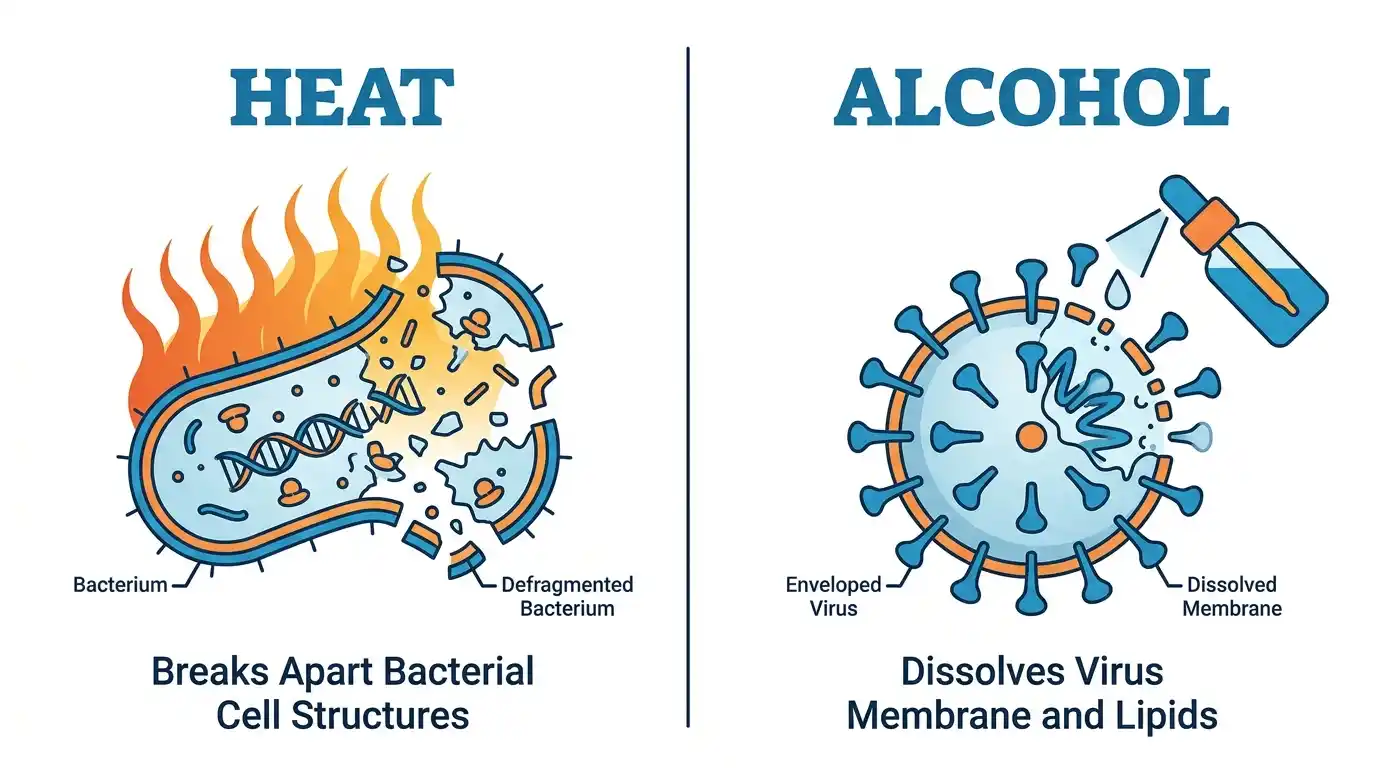
Heat and alcohol both affect the basic biology of bacteria, although they do so in distinct ways.
When bacteria and viruses get too hot, the proteins inside them denature, which means they stop working and fall apart. The bacterium can’t replicate or infect once those proteins are gone. It’s like taking the engine out of a car.
Alcohol acts by breaking down the lipid (fat) layer that surrounds most bacteria and viruses that are covered by a membrane, like influenza and SARS-CoV-2. The organism breaks down after that outer layer is gone. This is why hand sanitizers with alcohol in them became so popular during the COVID-19 outbreak.
Some germs, particularly non-enveloped viruses (norovirus, for example), are harder to kill with alcohol. That’s one reason why heat sterilization is still important: it kills germs that alcohol doesn’t.
What Surfaces Can Heat and Alcohol Not Be Used On?
Not every piece of equipment can safely go through heat or alcohol treatment. Understanding these limits is important.
Heat limitations: Plastic components, rubber seals, and electronic equipment don’t tolerate high temperatures. Items with batteries, screens, or delicate circuitry can’t go into an autoclave. Flexible endoscopes are a classic example steam damages them.
Alcohol limitations: Alcohol can degrade certain rubbers, acrylics, and some plastics over repeated use. It’s also ineffective against bacterial spores (like Clostridioides difficile), which need higher-level disinfectants or heat sterilization.
For equipment that falls into these categories, alternative types of disinfectant are used such as hydrogen peroxide vapor, glutaraldehyde, or UV light systems.
Common Hospital Equipment That Uses Heat and Alcohol
Here’s a quick breakdown of what gets treated with each method:
Heat Sterilization:
- Surgical scissors and scalpels
- Forceps and clamps
- Reusable syringes and needles (where applicable)
- Surgical drapes (some types)
- Metal dental tools
Alcohol Disinfection:
- Stethoscopes
- Blood pressure cuffs
- Thermometers
- Bedside tables and bed rails
- IV prep sites on patient skin
- Glucometers and monitoring devices
Some equipment gets both. A surgical tool might be autoclaved after use, then wiped with alcohol at the point of care between patients in an emergency.
Why This Matters in Home Care Settings
This isn’t just a hospital conversation. Anyone managing medical equipment at home whether caring for an elderly parent or recovering from surgery needs to understand basic disinfection principles too.
At Castle Pines Home Care, proper hygiene around medical equipment is part of every care plan. Whether it’s maintaining clean respiratory equipment or handling wound care tools safely, the same principles apply. If you’re looking for Home Care in Denver or need Medical Equipment Support Services in Denver, understanding why heat and alcohol are used to disinfect medical equipment helps you ask the right questions and make smarter choices for the people in your care.
Final Thoughts
The question of why heat and alcohol are used to disinfect medical equipment boils down to a balance of power and practicality. Heat provides the deep, total kill needed for invasive surgery, while alcohol provides the quick, everyday protection needed for surfaces and skin. By knowing when to use which, you’re protecting yourself and your loved ones from the invisible threats of the microbial world. If you have more questions about maintaining a safe environment or need professional assistance with your care needs, please feel free to contact us today to speak with one of our specialists. Stay safe, stay clean, and always double-check those equipment labels.
Frequently Asked Questions
Why do people use alcohol to clean instead of only water?
Water by itself doesn’t destroy germs; it just transports them around. Water can’t break down microbial cell membranes like alcohol does. That’s why alcohol is commonly used in medicine to clean surfaces.
What is the best concentration of alcohol for disinfecting medical equipment?
70% isopropyl alcohol is the most effective. Concentrations above 90% evaporate too quickly to work properly, while those below 60% may not kill enough pathogens reliably.
Does alcohol kill fungus on medical equipment?
Yes. Alcohol is effective against many fungal organisms, including Candida species. However, for heavy fungal contamination or spore-forming organisms, stronger disinfectants or heat sterilization may be needed.
Can you use rubbing alcohol on all medical equipment?
No. Alcohol can damage rubber, certain plastics, and acrylic surfaces with repeated use. Always check the manufacturer’s guidelines before applying alcohol to any piece of equipment.
What’s the difference between disinfection and sterilization?
Disinfection reduces pathogens to a safe level but may not eliminate all spores. Sterilization (typically via heat) destroys all microbial life, including spores. The method chosen depends on the risk level of the equipment’s use.
Is heat sanitizing better than alcohol?
It depends on the situation. Heat sanitizing is more thorough and handles a wider range of pathogens including spores. Alcohol is faster and more practical for surfaces that can’t be autoclaved. Most healthcare settings use both, depending on the equipment type.